Evolocumab enables rapid LDL-C reduction and inflammatory modulation during in-hospital stage of acute coronary syndrome: A pilot study on Chinese patients
Source : https://www.frontiersin.org/articles/10.3389/fcvm.2022.939791/full
Background and aimsProprotein convertase subtilisin/kexin type 9 (PCSK9) has long been considered a key regulator in lipid metabolism. Its role as a potential player in immune response has recently earned much attention.
Conclusions: In this case-crossover study of the effect of PCSK9 antibody among Chinese patients, evolocumab on top of high-intensity statin during hospitalization led to a remarkable and rapid reduction in atherogenic lipids and an alteration in inflammatory status at early-stage post-ACS.





• Source: Frontiers in Cardiovascular Medicine
• Conclusion: “In this case-crossover study of the effect of PCSK9 antibody among Chinese patients, evolocumab on top of high-intensity statin during hospitalization led to a remarkable and rapid reduction in atherogenic lipids and an alteration in inflammatory status at early-stage post-ACS [acute coronary syndrome].”
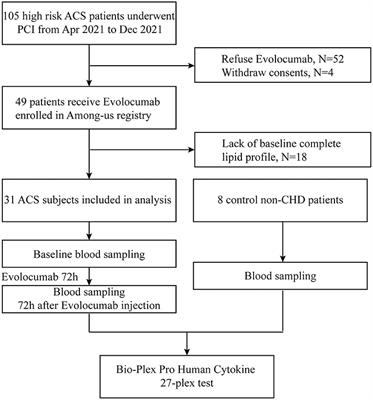
• In the current study, Chinese researchers analyzed the effects of evolocumab (140 mg) on lipid reduction in 31 inpatients hospitalized secondary to ACS vs 8 matched patients in the control group. The investigators administered one dose of subcutaneous evolocumab (140 mg) plus 10 mg/day rosuvastatin while patients were in the hospital. Serum levels of lipid and cytokines were also assessed.
• In addition to lowering LDL-C levels within 72 hours, evolocumab plus high-intensity statins led to a decrease in the circulating levels of the pro-inflammatory cytokines IL-1β, IL-6, and MCP-1; anti-inflammatory cytokines, including IL-13 and IL-4; and growth factors, including as GM-CSF and VEGF.
• To date,” the authors wrote, “the lipid management strategy for patients with ACS is stepwise and characterized by the initiation of high-intensity statin, succeeded by the addition of ezetimibe, and the administration of PCSK9 inhibitors only when the LDL-C level remains above the threshold . Following this approach, PCSK9 inhibitors would not be considered until several months after an index event. However, the risk of recurrent ischemic events remains the highest during early post-ACS probably because of the continued elevation of LDL-C level and overwhelming inflammation. Thus, a rapid lipid-lowering and inflammation-controlling approach is of great importance during acute-phase post-ACS.”
• Limitations of the current trial include its low power and lack of placebo for comparison. Furthermore, it’s unclear the effect that high-intensity statins had on findings; patients were taking high-intensity statins throughout their hospitalization.