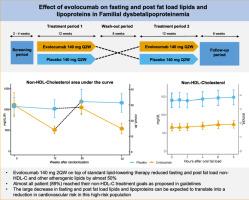
Effect of evolocumab on fasting and post fat load lipids and lipoproteins in familial dysbetalipoproteinemia
Source : https://www.lipidjournal.com/article/S1933-2874(22)00291-4/fulltext
Familial dysbetalipoproteinemia (FD), also known as 'remnant removal disease', is the second most common monogenic lipid disorder after heterozygous familial hypercholesterolemia (heFH), with an estimated prevalence of 1 in 850 to 1 in 3500 individuals.1 In clinical practice, FD is often not recognized and therefore underdiagnosed.
Conclusions: Evolocumab added to standard lipid-lowering therapy significantly reduced fasting and absolute post fat load concentrations of non-HDL-C, apoB and other atherogenic lipids and lipoproteins in FD patients. The clinically significant decrease in lipids and lipoproteins can be expected to translate into a reduction in CVD risk in these high-risk patients.





• Source: Journal of Clinical Lipidology
• Conclusion: “Evolocumab added to standard lipid-lowering therapy significantly reduced fasting and absolute post fat load concentrations of non-HDL-C, apoB and other atherogenic lipids and lipoproteins in FD [familial dysbetalipoproteinemia] patients. The clinically significant decrease in lipids and lipoproteins can be expected to translate into a reduction in CVD risk in these high-risk patients.”
• In this randomized placebo-controlled double-blind crossover trial, Dutch researchers compared the effects of evolocumab (140 mg SQ q2w) vs. placebo during two 12-week treatment periods in 28 patients with familial dysbetalipoproteinemia (FD).
• “In FD patients, LDL and LDL-cholesterol (LDL-C) levels are generally low or even absent, and thus do not adequately reflect CVD risk,” the authors stated. “Also, LDL-C levels cannot be measured accurately and therefore should not be measured in FD. Therefore, treatment goals for patients with FD are based on non-HDL-C levels. Medical treatment with diet, statins, and optionally fibrates, are recommended to achieve non-HDL-C treatment goals. However, in clinical practice 60% of FD patients do not achieve non-HDL-C treatment goals, even with optimal therapy, indicating the need for more intensive lipid-lowering treatment.”
• One limitation of the current study is that lipid levels were measured up to 8 hours following oral fat load, which may not be enough time to reflect post fat load response in FD patients.